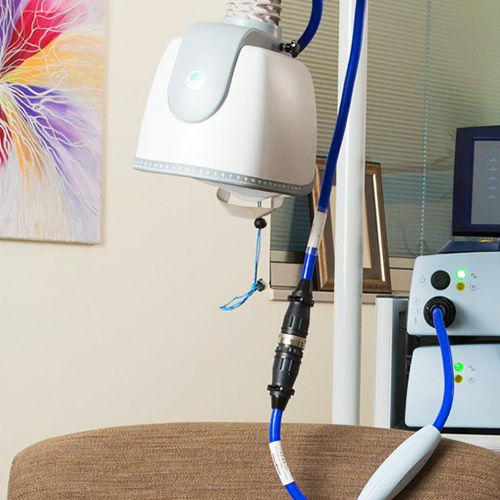
Transcranial Magnetic Stimulation sessions last approximately 18 minutes each and take place in a comfortable setting. TMS uses magnetic waves to activate certain areas of the brain.
During a TMS session, patients do not require anesthesia. An electromagnetic coil is placed against the patient’s forehead, and small, electromagnetic pulses are generated through the coil.
The pulses pass through the skull and stimulate the area of the brain thought to regulate mood.
Getting a TMS Appointment
Before you can sit down for TMS treatment, you will need to meet with a psychiatrist to determine the right treatment for you. If you haven’t experienced a full remission from antidepressants or psychotherapy, TMS can be employed as an alternative treatment, or to compliment antidepressant medications or psychotherapy. To make an appointment with our psychiatrist, click here.
Be sure to inform your treatment team of the following:
- If you’re taking any medications
- If you have had seizures before
- If you have any other mental health disorders
- If you received brain damage from an illness or injury
- If you suffer from frequent or severe headaches
- If you suffer from any other medical condition
What does it feel like?
For the next 18 minutes, you’ll feel pulses from the TMS coil that are delivered in 30-second intervals. People describe them as like a tapping on the scalp. The earplugs come in handy at this point to mask the clicking noise. They will be provided by the technician.
About one-third of patients may experience scalp sensations with TMS pulses. Patients tend to acclimate over the course of treatment, although adjustments can be made to reduce discomfort.
TMS therapy is focused and can be used to target exact locations, such as the Dorsolateral Prefrontal Cortex (DLPFC), where it can be used to deliver magnetic pulses.
How do you know it’s working?
- Fewer depressive symptoms
- Better sleep
- Better concentration
People often report feeling 70%-80% “more normal” after four to five weeks – and at six weeks, a lot of patients state that the majority of depressive symptoms have vanished.
Side Effects
Some patients report a light headache or discomfort from where the coil was placed but this can be remedied with over-the-counter pain medication and should go away soon. In fact, you can take medication thirty minutes before the procedure even begins to prevent the pain in the first place. If, however, pain persists, your doctor can reduce the magnetic field strength on your next session.
Fewer than five percent of patients discontinue TMS treatment because of pain or discomfort. In fact, there have been over 17,000 treatments under clinical trials, all of which were performed safely. No side effects such as weight gain, sexual problems, stomach issues, sleepiness, or dry mouth were reported.
Those same clinical trials point to most patients experiencing results by the fourth week – of course, some experience it sooner and some later, but a month seems to be the average. You’ll also see a visual picture of your progress via a depression inventory which is charted on a graph as you move through the treatment.
Overall, people undergoing TMS therapy saw an average drop in their depression symptom score of 22.1% – which is well over double to the 9% average reduction people not undergoing TMS see.
Long Term
If you are one of the few who does not see relief, your TMS sessions can be lengthened up to twelve weeks. Patients who report that TMS doesn’t work as well generally have either:
- Mental illness that includes detachment from reality (i.e., psychotic symptoms).
- Depression that’s already lasted several years.
- Already tried electroconvulsive therapy before that didn’t work.
Retreatment
Getting maintenance TMS treatment has been reported to be helpful for some patients. These booster cycles can sometimes be done 6 months or a year later. Each treatment plan is customized and it’s best to schedule a consultation with our psychiatrist.
Efficacy Rates
Over 3,500 papers have been published speaking to the efficacy of TMS. One report in particular performed at Butler Hospital by Dr. Linda Carpenter and her team discovered that TMS aided people who had treatment-resistant depression. They saw a 58% positive response rate and a 37% remissions rate.
Another trial in 2010 showed that TMS led to a 14% remission rate compared to 5% without it. A second phase of the trial allowed all patients – including those who’d received placebo versions of TMS – to receive proper TMS and, astonishingly, remission rates rose to almost 30%.
Of the patients who’ve claimed improvement from TMS, most state the benefits are still there three years later. TMS has a rich history of success and an abundance of evidence to prove it.
Let's Discuss Treatment Options.



